Diabetes is a serious chronic metabolic disease, which persists for life once manifested. It is characterized with an increased level of glucose in the blood, I.e. increased blood sugar level, due to lowered level or lack of insulin hormone or even a changed response of the body cells to insulin. Diabetes causes pathological disorders in the nervous system and in the blood vessels, which result in a number of disorders in different organs and systems.

Metabolism is the way by which substances exchange is carried out. It is responsible for the absorption of food sources in the body. Part of the food is metabolized to glucose – a monomeric carbohydrate, which is also the main energy source in the body. Insulin is a hormone secreted by the pancreas – it is responsible for the blood glucose assimilation. With the help of insulin blood glucose is injected into the cells of the body, which leads to a decrease in the level of glucose in the blood, I.e. a decrease in blood sugar. Once injected into body cells, glucose becomes an energy source for them and is a vital component in different metabolic paths.
If pathology is absent, insulin increases its level in an adequate amount after eating, when the level of glucose in the blood is increased, so that this glucose can be absorbed by the cells. This way, the level of glucose in the blood decreases, which is followed by decreasing blood insulin level respectively. If you have prediabetes or diabetes, blood sugar level remains high as a result of 2 causes: pancreas does not secrete sufficient amount of insulin, or the cells of the body have become insensitive to it, therefore increased blood glucose cannot be absorbed. Part of the glucose is excreted in the urine, which gives the name diabetes mellitus – the Greek word “diabanein” means a siphon, later changed into diabetes and “mellitus” – word from а Latin root, meaning honey. Urination becomes more frequent and the urine acquires a specific sweetish odor, similar to honey.
Types of diabetes
Тhere are 2 main types of diabetes:
Type 1 diabetes – also known as insulin-dependent, early or juvenile diabetes. It affects 10% of the diseased and manifests itself at an early age, before 40 years, often during puberty. Type 1 diabetes is characterized by reduced or absent insulin production by the pancreas. It is an autoimmune disease and develops when the insulin-producing cells in the pancreas are destroyed, causing glucose to remain in the bloodstream. This raises sugar levels in the blood which cannot be naturally corrected. Thus, type 1 diabetes require lifelong therapy with insulin and maintaining a healthy diet, accompanied by appropriate physical activity. If the diseased have no access to insulin, they can not survive.
Type 2 diabetes – also known as non-insulin-dependent diabetes mellitus. It affects 90% of the diseased, most often manifested at an older age. As the age passes by, the risk of developing this type of diabetes grows. Type 2 diabetes is characterized by reduced sensitivity of the body cells to insulin (insulin resistance) or an insufficient amount of insulin secretion.
Type 2 diabetes is a progressive disease with worsening symptoms. Vital to slowing the progression is the control of body weight and the maintenance of a healthy lifestyle, which combines rational nutrition and adequately increased physical activity. Monitoring blood sugar level daily is also necessary.
Obesity is the key factor for development and progression of this type of diabetes. The increased amount of visceral fat and abdominal fat leads to releasing of a large number of compounds from them with harmful effects on the cardiovascular system, which additionally slows metabolism.
The third type of diabetes, called gestational diabetes,is also known. It occurs in some women during pregnancy, which becomes a cause for the birth of larger babies. This type of diabetes most often resolves after pregnancy. During pregnancy, however, it is necessary to maintain a healthy lifestyle, especially rational nutrition. In some cases, medical therapy is also applied.
Risk factors
Statistics show that 1 of every 11 people suffers from diabetes, i.e. it is an extremely common disease. Which are the risk factors and how can we protect ourselves?
-Overweight and over-the-top body weight. The more fat you have, the more resistant body cells become to insulin.
– -Decreased physical activity. Physical activity contributes to nutrient absorption as an energy source, thus they are not stored as additional energy reserved in the form of fat. This way, optimal body weight is maintained and body cells become more sensitive to insulin.
– -Family encumbrance. he risk of developing diabetes is increased if a parent or relatives suffer from type 2 diabetes.
– -Elevated blood pressure. Blood pressure equal to or over 140/90 mm Hg is associated with an increased risk of developing type 2 diabetes.
– – Abnormal levels of cholesterol and triglycerides. Lower levels of “good cholesterol”, as well as elevated triglyceride levels, are associated with an increased risk of developing a type 2 diabetes. Lipid profile can be monitored by your doctor.
– – Lack of sleep. Insufficient rest and lack of sleep lead to a slowing of metabolism and metabolic processes disorders that affect carbohydrate and lipid profile.
– – Polycystic ovary syndrome Polycystic ovary syndrome is a common condition in women, which is characterized by irregular menstrual periods, accelerated hair growth and obesity, that increases the risk of type 2 diabetes.
Complications
The more time you suffer from diabetes, the more difficulties appear in controlling blood sugar level – therefore, the progression of complications is also observed. Possible complications are:
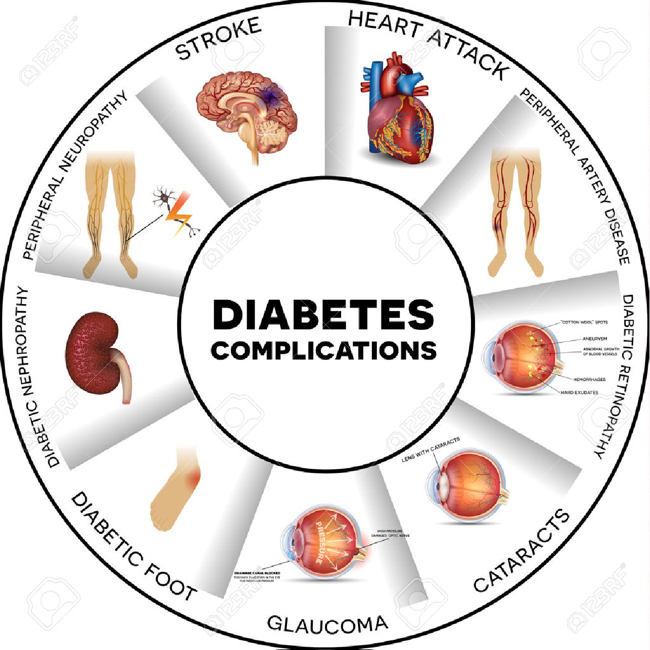
– Cardiovascular disorders. Diabetes is associated with an increased risk of cardiovascular system disorders such as atherosclerosis (narrowing of the arterial vessels), heart failure, stroke etc.
– – Neuropathy (nerve damage). The increased amount of blood sugar can damage capillary walls (tiny blood vessels), which are responsible for nerves supply of nutrients, especially in the area of lower limbs. This can cause a feeling of pain, numbness with subsequent loss of sensitivity. Most often, pain begins in the finger area of lower limbs, progressively spreading to upper parts of limbs.
If neuropathy affects nerves associated with digestion, this can lead to digestive disorders such as nausea, vomiting, diarrhea, etc. In men, neuropathy can lead to erectile dysfunction.
– – Nephropathy (kidney damage). The kidneys are replete of millions of clusters of small blood vessels called glomerules, which are responsible for blood filtration. The increased amount of blood sugar can lead to their damage, similar to the damage in neuropathy. This condition can lead to severe renal disorders associated with kidney failure, including end-stage renal damage, which requires hemodialysis, even kidney transplantation.
-Retinopathy (damage to the visual system). Increased blood sugar levels can cause damage to blood vessels supplying the retina (diabetic retinopathy). Progression of the injury can lead to blindness. In addition, diabetes can also cause other visual disturbances such as glaucoma, cataracts, etc.
– -Skin disorders Diabetes can lower the immunity of the largest barrier in the body – the skin. Skin becomes more susceptible to bacterial and fungal infections.
– -Injuries of lower limbs. Decreased blood supply of lower limbs or nerve damage of lower limbs may lead to an increased risk of infections in the are. If left untreated, complications become more complex to treat, thus this could lead to amputation of fingers, foot, even of the whole limb.
-Hair loss.
-Risk of developing Alzheimer’s disease. The more the blood sugar level increases, the higher the risk of developing dementia, incl. Alzheimer’s disease. These are still only theories and no scientific justification exists for the relationship between type 2 diabetes and dementia.
– – Depression. Due to the development of various complications, depression is a common condition among sufferers of type 1 diabetes and type 2 diabetes. Depression in turn can complicate the management of the disease.
Prevention.
How to outsmart diabetes? The choice of a healthy lifestyle associated with changing some habits can become a secret weapon for prevention from developing diabetes or prevention from complications if the condition of prediabetes or diabetes is already present.

– Healthy eating. The choice of organic foods, which are richer in vitamins and minerals and lower in calorific value rather than choosing junk semi-finished products, is a great start for a weight loss program and for maintaining body health. Strive for foods rich in fibers, low in fat and low in calories. Choose vegetables, an adequate amount of fruits, whole grains. Strive for diverse and rational diet.

– -Increased physical activity. Increased physical activity = increased energy consumption = weight reduction + increased muscle tone + improved emotional state.
– – Weight reduction. It has been scientifically proven that losing only 7% of body weight can significantly reduce the risk of developing diabetes.
Weight loss should not be associated with inconsistent lifestyle changes, of course. Weight reduction is healthy when it happens gradually and it is associated with lifelong changes in food choices and physical activity habits.
Drug therapy is also important for maintaining health and prevention from complications in prediabetes and diabetes. However, it must always be accompanied with healthy habits in order to be as effective as possible.
How to recognize diabetes if it has already appeared?
Initially, the symptoms of diabetes are harmless and sometimes even imperceptible. It is of great importance to follow the changes in our physiological state to understand when we have a health problem – prediabetes, diabetes or other condition.
Which are the symptoms that should lead us to the doctor’s door?
– -Frequent urination. Increased blood sugar level with decreased absorption leads to excretion of glucose through the urine, the urine is characterized by a specific sweet odor. Urine, rich in glucose, draws an increased amount of water, as the kidneys need more water to dilute the excreted glucose. This leads to a faster filling of the bladder and a more frequent urge to urinate
– -Increased thirst. Frequent urination leads to dehydration, which leads to increased thirst. Even drinking more fluids, however, the thirst still remains.
– -Increased hunger. When glucose absorption is reduced, a sufficient amount of energy source is not in the cells. Regardless of the elevated levels of blood glucose, received through food, the body feels a shortage of energy, which leads to constant hunger because of body cell shortage of energy.
– – Weight gain. Due to constant hunger and increased energy consumption, weight gain is often observed.
– Abnormal weight loss in type 1 diabetes, sometimes in diabetes type 2 Weight loss is triggered by the breakdown of muscles, which serve as a source of glucose after metabolic transformations – a method of survival of the organism.
– -Blurred vision.
-Delayed wound healing.
– Irritability.
– Chronic fatigue.
– Numbness and tingling in the limbs.
– etc.
Sources:
- www.who.int
- www.puls.bg
- www.mayoclinics.org
- www.News-Medical.net
- www.everydayhealth.com